There are a plethora of masks around, homemade as well as store bought. The range of effectiveness is vast. The Journal of the American Medical Association (JAMA) suggests that face shields may be a worthwhile alternative.
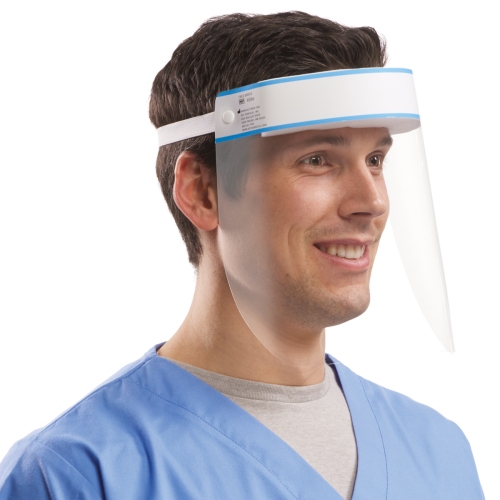
Face shields come in various forms, but all provide a clear plastic barrier that covers the face. For optimal protection, the shield should extend below the chin anteriorly, to the ears laterally, and there should be no exposed gap between the forehead and the shield’s headpiece. Face shields require no special materials for fabrication and production lines can be repurposed fairly rapidly. Numerous companies, including Apple, Nike, GM, and John Deere, have all started producing face shields. These shields can be made from materials found in craft or office supply stores. Thus, availability of face shields is currently greater than that of medical masks.
Face shields offer a number of advantages. While medical masks have limited durability and little potential for reprocessing, face shields can be reused indefinitely and are easily cleaned with soap and water, or common household disinfectants. They are comfortable to wear, protect the portals of viral entry, and reduce the potential for auto-inoculation by preventing the wearer from touching their face. People wearing medical masks often have to remove them to communicate with others around them; this is not necessary with face shields. The use of a face shield is also a reminder to maintain social distancing, but allows visibility of facial expressions and lip movements for speech perception.
Most important, face shields appear to significantly reduce the amount of inhalation exposure to influenza virus, another droplet-spread respiratory virus. In a simulation study, face shields were shown to reduce immediate viral exposure by 96% when worn by a simulated health care worker within 18 inches of a cough. Even after 30 minutes, the protective effect exceeded 80% and face shields blocked 68% of small particle aerosols,10 which are not thought to be a dominant mode of transmission of SARS-CoV-2. When the study was repeated at the currently recommended physical distancing distance of 6 feet, face shields reduced inhaled virus by 92%, similar to distancing alone, which reinforces the importance of physical distancing in preventing viral respiratory infections. Of note, no studies have evaluated the effects or potential benefits of face shields on source control, ie, containing a sneeze or cough, when worn by asymptomatic or symptomatic infected persons. However, with efficacy ranges of 68% to 96% for a single face shield, it is likely that adding source control would only improve efficacy, and studies should be completed quickly to evaluate this.
Major policy recommendations should be evaluated using clinical studies. However, it is unlikely that a randomized trial of face shields could be completed in time to verify efficacy. No clinical trial has been conducted to assess the efficacy of widespread testing and contact tracing, but that approach is based on years of experience. Taken as a bundle, the effectiveness of adding face shields as a community intervention to the currently proposed containment strategies should be evaluated using existing mathematical models. The implicit goal of face shields alone or in combination with other interventions should be to interrupt transmission by reducing the R0 to less than 1. Notably, effective control of even the most infectious pathogens, such as measles, does not require a vaccine with 100% efficacy. No burden of 100% efficacy should be placed on face shields or any containment policy because this level of control is both impossible to achieve and unnecessary to drive SARS-CoV-2 infection levels into a manageable range.
Conclusions
The COVID-19 pandemic arrived swiftly and found many countries unprepared. Even highly prepared countries are now facing second-wave outbreaks that have forced implementation of extreme social distancing measures. To minimize the medical and economic consequences, it is important to rapidly assess and adopt a containment intervention bundle that drives transmissibility to manageable levels. Face shields, which can be quickly and affordably produced and distributed, should be included as part of strategies to safely and significantly reduce transmission in the community setting. Now is the time for adoption of this practical intervention.







